Palliative Care for Geriatric Trauma Patients, Trauma Center Care and Routine Processes for Care - Evidence-Based Review
Published 2019
Citation: J Trauma. 86(4):737-743, April 2019
Evidence-based review of trauma center care and routine palliative care processes for geriatric trauma patients; A collaboration from the American Association for the Surgery of Trauma Patient Assessment Committee, the American Association for the Surgery of Trauma Geriatric Trauma Committee, and the Eastern Association for the Surgery of Trauma Guidelines Committee
Authors
Aziz, Hiba Abdel, MD; Lunde, John, DNP; Barraco, Robert, MD, MPH; Como, John J., MD, MPH; Cooper, Zara, MD, MSc; Hayward, Thomas III, MD; Hwang, Franchesca, MD, MSc; Lottenberg, Lawrence, MD; Mentzer, Caleb, DO; Mosenthal, Anne, MD; Mukherjee, Kaushik, MD, MSci; Nash, Joshua, DO; Robinson, Bryce, MD, MS; Staudenmayer, Kristan, MD, MS; Wright, Rebecca, PhD; Yon, James, MD; Crandall, Marie, MD, MPH
Author Information
From the Northeastern Ohio University (H.A.A.), Rootstown, Ohio; Orange Park Medical Center (J.L.), Orange Park, Florida; Lehigh Valley Health Network (R.B.), Allentown, Pennsylvania; MetroHealth Medical Center (J.J.C.), Cleveland, Ohio; Harvard University (Z.C.), Cambridge, Massachusetts; Indiana University (T.H.); Rutgers–New Jersey Medical School (F.H., A.M.), Newark, New Jersey; Florida Atlantic University (L.L.), Boca Raton, Florida; Augusta University (C.M.), Augusta, Georgia; Loma Linda University Medical Center (K.M.), Loma Linda, California; Summa Health (J.N.), Akron, Ohio; University of Washington (B.R.), Seattle, WA; Stanford University (K.S.), Stanford, California; Johns Hopkins University (R.W.), Baltimore, MD; Sky Ridge Surgical Center (J.Y.), Lone Tree, Colorado; and University of Florida College of Medicine (M.C.), Jacksonville, Florida.
Submitted: August 20, 2018, Revised: October 18, 2018, Accepted: November 14, 2018, Published online: December 10, 2018.
Address for reprints: Marie Crandall, MD, MPH, FACS, University of Florida College of Medicine Jacksonville, 655 W 8th St, Jacksonville, FL 32209; email: marie.crandall@jax.ufl.edu.
BACKGROUND Despite an aging population and increasing number of geriatric trauma patients annually, gaps in our understanding of best practices for geriatric trauma patients persist. We know that trauma center care improves outcomes for injured patients generally, and palliative careprocesses can improve outcomes for disease-specific conditions, and our goal was to determine effectiveness of these interventions on outcomes for geriatric trauma patients.
METHODS A priori questions were created regarding outcomes for patients 65 years or older with respect to care at trauma centers versus nontrauma centers and use of routine palliative careprocesses. A query of MEDLINE, PubMed, Cochrane Library, and EMBASE was performed. Letters to the editor, case reports, book chapters, and review articles were excluded. GRADE (Grading of Recommendations Assessment, Development and Evaluation) methodology was used to perform a systematic review and create recommendations.
RESULTS We reviewed seven articles relevant to trauma center care and nine articles reporting results on palliative care processes as they related to geriatric trauma patients. Given data quality and limitations, we conditionally recommend trauma center care for the severely injured geriatric trauma patients but are unable to make a recommendation on the question of routine palliative care processes for geriatric trauma patients.
CONCLUSIONS As our older adult population increases, injured geriatric patients will continue to pose challenges for care, such as comorbidities or frailty. We found that trauma center care was associated with improved outcomes for geriatric trauma patients in most studies and that utilization of early palliative care consultations was generally associated with improved secondary outcomes, such as length of stay; however, inconsistency and imprecision prevented us from making a clear recommendation for this question. As caregivers, we should ensure adequate support for trauma systems and palliative care processes in our institutions and communities and continue to support robust research to study these and other aspects of geriatric trauma.
LEVEL OF EVIDENCE Systematic review/guideline, level III.
As the geriatric population in the United States increases, trauma centers (TCs) across the country are seeing more older trauma patients. Patients 65 years or older account for 20% of all hospital trauma-related admissions. Of trauma patients admitted to the intensive care unit (ICU) in this age group, 10% to 20% die of their injuries.[1] While older individuals comprise 20% of trauma patients, they require more costly care. More than 25% of total US trauma expenses are incurred by geriatric trauma patients. These patients present additional challenges that should be considered when planning care, including medical comorbidities, frailty, and impaired immune response to injury.[2]
In 2012, Calland et al[3] published an Eastern Association for the Surgery of Trauma Practice Management Guideline (EAST PMG) on geriatric trauma. The recommendations at that time were for aggressive triage practices, recognition and correction of coagulopathy, and early limitation of futile care, which have become standard practice. The American College of Surgeons has recognized the importance of geriatric trauma care, and their Trauma Quality Improvement Project group recently published guidelines with respect to many aspects of the care of elderly trauma patients, including discussions on patient decision-making capacity and anticoagulant therapy, among others.[4]
However, gaps in our understanding of best practices for geriatric trauma patients persist. For this reason, a multiorganizational team that comprised members from the American Association for the Surgery of Trauma Patient Assessment Committee, the American Association for the Surgery of Trauma Geriatric Trauma Committee, and the EAST Guidelines Committee convened to study 2 critical aspects of geriatric trauma, the benefits of TC versus non-TC care and the use of palliative care processes on outcomes for older trauma patients.
While the benefits of TC care for injured patients have been well described, specific benefits to elderly patients remain unclear. Similarly, although palliative care is becoming ubiquitous in the critical care setting, its impact on the trauma population has not been well reviewed. The framework for palliative carefocuses on quality of life as defined by the patient, with a strong emphasis on comfort at the end of life.[5]The optimal use and timing of palliative care for the older trauma patient have not been fully addressed.
As a final point, there is lack of unanimity with respect to the definition of “geriatric.” Trauma mortality seems to increase somewhere between the ages 55 and 65 years,[6] and the American College of Surgeons Committee on Trauma recommends consideration for triage to TCs for patients 55 years or older. However, much of the focused geriatric trauma literature uses age 65 years or even older when examining interventions. For this reason, we chose to focus on interventions targeting adults 65 years or older.
Objectives
The purpose of this review was to provide a systematic review of 2 key issues in care of the geriatric trauma patient: TC management and palliative care processes.
Process
We utilized the GRADE (Grading of Recommendations Assessment, Development and Evaluation) methodology.[7] The GRADE approach dictates a priori creation of questions in the Population, Intervention, Comparator, Outcome (PICO) format. The PICO questions to guide this systematic review were created using a modified Delphi method by the EAST Guidelines Committee Injury Prevention Task Force. We began by identifying areas of clinical interest for caregivers of geriatric trauma patients, topics that may inform decisions about trauma systems planning or care practices. Two of the areas where we felt guidelines might be helpful were utility of TC care for geriatric trauma patients and routine use of palliative care processes for geriatric trauma patients.
PICO Questions
PICO Question 1: Should geriatric patients receive postinjury care at a TC?
Population: Trauma patients 65 years or older
Intervention: Postinjury care at a TC
Comparator: Postinjury care at a non-TC
Outcomes: Mortality, discharge disposition, independence/long-term functional outcomes
PICO Question 2: Should geriatric trauma patients receive routine palliative care processes?
Population: Trauma patients 65 years or older
Intervention: Ordering and routine use of palliative care processes
Comparator: No routine ordering or use of palliative care processes
Outcomes: Mortality, discharge disposition, independence/long-term functional outcomes
Methods
Inclusion Criteria for This Review
Study Types
Studies included randomized controlled trials, prospective and retrospective observational studies, ecological studies, and case-control studies. Case reports, conceptual pieces, and reviews containing no original data or analyses were excluded. We excluded editorials, opinion articles, and studies not addressing the PICO questions. We included all studies published between January 1, 1900, and August 31, 2017. We did not restrict by publication language but excluded articles without an English translation.
Participant Types
We included all relevant studies, irrespective of race, sex, or other demographic characteristics.
Intervention Types
We reviewed all studies that compared outcomes for geriatric trauma patients at TCs versus non-TCs. Trauma centers were defined by the original investigators for each study and could be either state-verified and/or American College of Surgeons–verified centers. We also examined outcomes for routine versus no routine palliative care processes in our population of interest.
Outcome Measure Types
Many potential outcomes of interest were posited, including resource allocation, clinical outcomes, and hospital charges. Each person voted on each outcome based on a 10-point Likert scale to determine critical outcomes, which all had a mean score of 7 or higher. We limited the review to studies in which our critical outcomes were studied: mortality, discharge disposition, and independence/long-term functional outcomes.
Review Methods
Search Strategy

Figure 1. Search strategy.
In September 2017, an institutional research librarian performed a systematic search of Ovid, MEDLINE, EMBASE, and Web of Science. Figure 1 contains the MeSH terms used for the initial search.
Study Selection
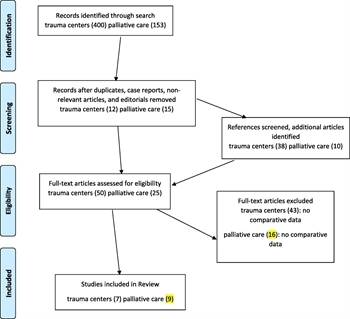
Figure 2. PRISMA flow diagram.
Two independent reviewers (H.A.A., M.C.) screened the references by title and abstract, and all nonrelevant articles, editorials, case reports, and duplicates were removed. We then screened references for each article and added pertinent articles to the total. The resulting studies were used for this review. The study selection process is highlighted in the PRISMA flow diagram in Figure 2.
A total of 400 abstracts were identified in our initial searches for PICO 1, and 153 abstracts were identified for PICO 2. Duplicates, case reports, articles not relevant to the PICO questions, and editorials were excluded, leaving 12 articles applicable to PICO 1 and 15 for PICO 2. We then reviewed the references for these articles and screened an additional 38 articles for PICO 1 and 10 for PICO 2. Finally, the full articles were reviewed for relevance, and we excluded articles that did not include comparative data. Our final list comprised seven articles for PICO 1 and nine for PICO 2.
Data Extraction and Management
All references used for the review were loaded onto a Google Drive (Google LLC, Menlo Park, CA). All articles, GRADE resources, and instructions were electronically available to all members of the writing team. Each independent reviewer shared his or her PICO sheet and literature review with all members of the team. Independent interpretations of the data were shared through group email and conference calls. No reviewer discrepancies occurred. Grading was completed in January 2018.
Methodological Quality Assessment
We used the validated GRADE methodology for this study.[7] The GRADE methodology entails the creation of a predetermined PICO question or set of PICO questions that the literature aims to answer. Each designated reviewer independently evaluates the data in aggregate with respect to the quality of the evidence to adequately answer each PICO question and quantified the strength of any recommendations. Reviewers are asked to determine effect size, risk of bias, inconsistency, indirectness, precision, and publication bias.
Recommendations are based on the overall quality of the evidence. GRADE methodology suggests the phrases “we recommend” for strong evidence and “we conditionally recommend” for weaker evidence.
Results
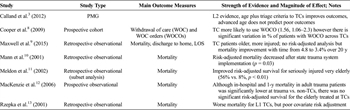

Table 1. PICO 1: Trauma Centers and Geriatric Trauma Outcomes

Table 2. PICO 2: Palliative Care and Geriatric Trauma Outcomes
Seven articles met inclusion criteria for PICO 1 (Table 1), and nine articles were relevant for PICO 2 (Table 2). Our results provide a summary overview of the articles and key strengths and weaknesses.
PICO 1: Should Geriatric Patients Receive Postinjury Care at a Trauma Center?
For PICO 1, we found seven observational studies that compared the outcomes of severely injured geriatric trauma patients between TCs and non-TCs; all focused on mortality as their outcome of interest; one also examined discharge disposition, but none described long-term functional outcomes/independence.
Mann et al.[10] assessed the impact of implementation of a statewide trauma system on the survival of injured elders. This allowed for an indirect pre/post comparison of TCs and trauma systems. Survival of severely injured geriatric patients (Injury Severity Score [ISS] >15) improved by 5.1% (p = 0.03) after implementation, without improvement in survival of nontrauma patients during the study period. Meldon et al.[11] examined the relationship between TC verification and hospital mortality in very old (>80 years) trauma victims. Risk-adjusted survival for the severely injured patients (ISS 21–45) in this cohort was significantly better in TCs versus non-TCs (56% vs. 8%; p < 0.01).
Maxwell et al.[9] compared national data obtained in 2009 with data from 1989, analyzing more than 25,000 records. Despite a steady rise in the percentages of patients in the older age groups, the overall percentage of deaths declined from 4.8% to 3.4% over 20 years. They found that Level I trauma centers admitted more severely injured patients and had higher mortality rates than Level II/III/IV TCs or non-TCs, but no multivariate analysis to adjust for risk was performed. In another national study using the National Study on Costs and Outcomes of Trauma, MacKenzie et al.[12] examined mortality differences between Level I TCs and non-TCs in adult patients aged 18 to 84 years with moderate to severe injuries. In this study, the in-hospital mortality rate was sizably lower at TCs than at non-TCs (7.6% vs. 9.5%; relative risk, 0.80), as was the 1-year mortality rate (10.4% vs. 13.8%; relative risk, 0.75). However, the effect of treatment at a TC was only statistically significant for patients younger than 55 years, but not for those 55 years or older.
Rzepka and colleagues[13] found that Level I TC patients suffered greater inpatient mortality (odds ratio, 1.49; 95% confidence interval, 1.43–1.55) even when controlling for age, gender, race, and having multiple trauma diagnoses. However, commonly used metrics to risk stratify injury severity, such as the ISS, Glasgow Coma Scale score, or physiologic variables such as hypotension and requirement for blood transfusion were not included in the analysis. The authors noted that in addition to other confounding factors Level I TCs admitted a more severely injured geriatric population. In 2009, Cooper et al.[8] reported that TCs were more likely to use withdrawal of care orders than non-TCs, which may partly explain mortality differences. Finally, the 2012 EAST PMG determined that there was strong evidence to support triage of geriatric trauma patients, particularly the very old and those with preexisting medical conditions, preferentially to TCs.[3] However, their recommendations were largely based on studies that examined the effects of field triage criteria and undertriage of geriatric trauma patients, as opposed to hospital-level comparative studies of patient outcomes.
In grading the above studies with respect to PICO 1, we reviewed seven observational studies; we noted a serious risk of bias, very serious inconsistency, and serious imprecision in the conclusions from these studies. However, particularly given the methodologic strength, population sizes, and effect sizes of the studies of Mann et al.[10] and Meldon et al.,[11] we conditionally recommend TC care for the severely injured geriatric trauma patients.
PICO 2: Should Geriatric Trauma Patients Receive Routine Palliative Care Processes?
For PICO 2, we found nine observational studies with some comparative clinical data between geriatric trauma patient cohorts. However, only four studies directly assessed mortality, and none assessed our other outcomes of interest. Despite these challenges, we present results of the literature review to provide an overview of our current understanding of the topic, irrespective of our PICO question.
In a retrospective observational study, Khandelwal and colleagues[1] simulated the costs of ICU-based palliative care interventions under different reimbursement models. They estimated the potential savings in the direct variable costs at $1,300 per patient and a length of stay (LOS) reduction by 1.7 days. In the long term, another $2,800 per patient in direct fixed costs could be saved. In a 2015 study, Kupensky et al.[15] further demonstrated the impact of palliative medicine consultations (PMCs) for geriatric traumapatients in aligning care with patient preferences. Patients were significantly more likely to discuss advance directives (documented at 93.1% vs. 6.9%; p < 0.001) and update or change code status (84.5% vs. 15.5%; p < 0.001) if they received a PMC. On average, time from admission to palliative consultation was 2.9 days (range, 0–15 days), with patients who received consults on or before hospital day 2 demonstrating a statistically significant reduction in both mean surgical ICU LOS (6.4 vs. 11.8 days; p < 0.001) and hospital LOS (7.9 vs. 13.1 days; p = 0.001) despite higher mean ISS (19.6 vs. 16.3; p = 0.015). Patients who received PMC were significantly older and had significantly higher injury severity scores and a higher mortality rate than patients who did not receive PMC.
Katrancha and Zipf[14] performed a retrospective study reviewing the utility of a virtual geriatric traumainstitute, which included routine palliative care processes, along with algorithms for care in a multidisciplinary pathway in a retrospective study. Preimplementation and postimplementation data were compared for LOS, length of time in the emergency department (ED), and ED to operating room time. Geriatric trauma institute guidelines helped expedite the care of the elderly and decreased LOS from 4.9 to 3.9 days (p = 0.001). However, this study examined bundled care practices, and it was unclear to what extent the palliative care interventions contributed to these results.
In 2008, Mosenthal et al.[18] performed a prospective, observational study in a trauma ICU aiming at providing support ascertaining prognosis and eliciting patient preferences on admission followed by interdisciplinary family meeting within 72 hours. They found that early discussions between physicians and families and integration of palliative care resulted in consensus around goals of care without adversely influencing life expectancy. In a later study, the authors further advocated a collaborative approach that includes all team members from the surgical, critical care, and palliative disciplines.[4] They emphasized that whether in a “consultative” or “integrative” model palliative care can be delivered simultaneously with aggressive care plans with no increase in ICU or hospital mortality.
Although Cooper et al.[8] noted that patients admitted to TCs are more likely to have withdrawal of care orders, Matsushima et al.[16] found no correlation between in-hospital mortality of patients with do-not-resuscitate (DNR) orders and trauma designation level, but a higher level of complications. The authors posited this may be due to more aggressive treatment practices as Level I centers, but it would need further study. In a 2013 study, McBrien et al.[17] found a paucity of end-of-life decision-making documentation in the orthogeriatric subpopulation without any clear associations with outcomes or risk factors.
For PICO 2, we reviewed nine observational studies. We found serious risks of bias, indirectness, and imprecision among the studies. Only four studies directly assessed mortality, and none assessed our other outcomes of interest: discharge disposition and independence/long-term functional status. The challenges to informed decision making following geriatric trauma have been highlighted in several previous studies.[19][20] Although well proven to decrease LOS and hospital costs without negatively impacting mortality in the ICU, palliative care for geriatric trauma patients does not yet have a solid evidence base for the metrics we studied, that is, mortality, discharge disposition, and functional outcomes. For these reasons, we cannot make a recommendation on the question of routine palliative care processes for geriatric trauma patients.
Discussion
Trauma affects more than 1 million Americans 65 years or older, and more than 40,000 die of their injuries.[21] Improved trauma outcomes have been clearly associated with organized trauma systems, including specialized TC care.[12] Additionally, palliative care discussions and consultations have been shown to decrease lengths of stay and improve care coordination for older adults in nontrauma settings.[22][23] Our goal with this evidence-based review was to determine the effect of TC care and routine palliative care practices on outcomes for geriatric trauma patients.
In studying these topics, we encountered several limitations: we found relatively weak data with no randomized controlled trials; lack of data specificity, particularly with respect to outcomes of interest such as long-term functional status; and the potential for bias given study design challenges. We also found no unanimity in the definition of elderly, which hampers study inclusion definitions; our use of the age 65 years was most common, but this may have impacted our findings. However, despite these limitations, most studies supported similar conclusions with at least a modest effect size, allowing us to make some recommendations for clinical practice.
Using These Guidelines in Clinical Practice

Table 3. Summary of Recommendations
As our older adult population increases, injured geriatric patients will continue to pose challenges for care, such as comorbidities or frailty. We found that TC care was associated with improved outcomes for geriatric trauma patients in most studies and that utilization of early palliative care consultations was generally associated with improved secondary outcomes, such as LOS (Table 3). As caregivers, we should ensure adequate support for trauma systems and palliative care processes in our institutions and communities and continue to support robust research to study these and other aspects of geriatric trauma.
Conclusions
After review of the available evidence regarding TC care and palliative care processes for older trauma patients, we found moderate associations with improved geriatric outcomes. Further updates and future studies should continue to define the likely benefits of TCs on outcomes for injured geriatric patients. Finally, the field of palliative care medicine is growing, and with time will come standard process measures to inform future research, and patient-centered outcomes such as functional independence are critical for optimal care of the geriatric trauma patient.
Authorship
M.C., B.R., R.B., Z.C., and A.M. designed this study. M.C. conducted the literature search. J.C., B.R., H.A., R.B., J.L., F.H., T.H., B.R., A.M., J.Y., K.M., L.L., C.M., R.W., and M.C. graded the evidence. M.C., B.R., J.C., and R.B. interpreted the data. H.A., J.L., and M.C. prepared the manuscript. M.C. edited the manuscript.
References
- Khandelwal N, Benkeser D, Coe NB, Engelberg RA, Teno JM, Curtis JR. Patterns of cost for patients dying in the intensive care unit and implications for cost savings of palliative care interventions. J Palliat Med. 2016;19(11):1171–1178.
- McKevitt EC, Calvert E, Ng A, Simons RK, Kirkpatrick AW, Appleton L, Brown DR. Geriatric trauma: resource use and patient outcomes. Can J Surg. 2003;46(3):211–215.
- Calland JF, Ingraham AM, Martin N, Marshall GT, Schulman CI, Stapleton T, Barraco R. Evaluation and management of geriatric trauma: an Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg. 2012;73(5 Suppl 4):S345–S350.
- American College of Surgeons Trauma Quality Improvement Project Geriatric Trauma Management Guidelines. 2012. Available at: https://www.facs.org/~/media/files/quality%20programs/trauma/tqip/geriatric%20guide%20tqip.ashx Accessed October 2018.
- Mosenthal AC, Weissman DE, Curtis JR, Hays RM, Lustbader DR, Mulkerin C, Puntillo KA, Ray DE, Bassett R, Ross RD, et al. Integrating palliative care in the surgical and trauma intensive care unit: a report from the Improving Palliative Care in the Intensive Care Unit (IPAL-ICU) Project Advisory Board and the Center to Advance Palliative Care. Crit Care Med. 2012;40(4):1199–1206.
- Morris JA Jr., MacKenzie EJ, Damiano AM, Bass SM. Mortality in trauma patients: the interaction between host factors and severity. J Trauma. 1990;30(12):1476–1482.
- Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, Schunemann HJ. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336(7650):924–926.
- Cooper Z, Rivara FP, Wang J, MacKenzie EJ, Jurkovich GJ. Withdrawal of life-sustaining therapy in injured patients: variations between trauma centers and nontrauma centers. J Trauma. 2009;66(5):1327–1335.
- Maxwell CA, Miller RS, Dietrich MS, Mion LC, Minnick A. The aging of America: a comprehensive look at over 25,000 geriatric trauma admissions to United States hospitals. Am Surg. 2015;81(6):630–636.
- Mann NC, Cahn RM, Mullins RJ, Brand DM, Jurkovich GJ. Survival among injured geriatric patients during construction of a statewide trauma system. J Trauma. 2001;50(6):1111–1116.
- Meldon SW, Reilly M, Drew BL, Mancuso C, Fallon W Jr. Trauma in the very elderly: a community-based study of outcomes at trauma and nontrauma centers. J Trauma. 2002;52(1):79–84.
- MacKenzie EJ, Rivara FP, Jurkovich GJ, Nathens AB, Frey KP, Egleston BL, Salkevar DS, Scharfstein DO. A national evaluation of the effect of trauma-center care on mortality. N Engl J Med. 2006;354(4):366–378.
- Rzepka SG, Malangoni MA, Rimm AA. Geriatric trauma hospitalization in the United States: a population-based study. J Clin Epidemiol. 2001;54(6):627–633.
- Katrancha ED, Zipf J. Evaluation of a virtual geriatric trauma institute. J Trauma Nurs. 2014;21(6):278–281.
- Kupensky D, Hileman BM, Emerick ES, Chance EA. Palliative medicine consultation reduces length of stay, improves symptom management, and clarifies advance directives in the geriatric trauma population. J Trauma Nurs. 2015;22(5):261–265.
- Matsushima K, Schaefer EW, Won EJ, Armen SB. The outcome of trauma patients with do-not-resuscitate orders. J Surg Res. 2016;200(2):631–636.
- McBrien ME, Kavanagh A, Heyburn G, Elliott JR. ‘Do not attempt resuscitation’ (DNAR) decisions in patients with femoral fractures: modification, clinical management and outcome. Age Ageing. 2013;42(2):246–249.
- Mosenthal AC, Murphy PA, Barker LK, Lavery R, Retano A, Livingston DH. Changing the culture around end-of-life care in the trauma intensive care unit. J Trauma. 2008;64(6):1587–1593.
- Toevs CC. Palliative medicine in the surgical intensive care unit and trauma. Surg Clin North Am. 2011;91(2):325–331, viii.
- O'Connell K, Maier R. Palliative care in the trauma ICU. Curr Opin Crit Care. 2016;22(6):584–590.
- Zafar SN, Obirieze A, Schneider EB, Hashmi ZG, Scott VK, Greene WR, Efron DT, MacKenzie EJ, Cornwell EE 3rd, Haider AH. Outcomes of trauma care at centers treating a higher proportion of older patients: the case for geriatric trauma centers. J Trauma Acute Care Surg. 2015;78(4):852–859.
- Haun MW, Estel S, Rücker G, Friederich HC, Villalobos M, Thomas M, Hartmann M. Early palliative care for adults with advanced cancer. Cochrane Database Syst Rev. 2017;6:CD011129.
- Brannstrom M, Boman K. Effects of person-centred and integrated chronic heart failure and palliative home care. PREFER: a randomized controlled study. Eur J Heart Fail. 2014;16(10):1142–1151.
Keywords:
Evidence-based medicine; geriatric trauma; palliative care; practice management guideline; trauma systems